Parkinson’s disease as a somato-cognitive action network disorder
2026-02-06

Hesheng Liu and his team have found a key brain function network that’s disrupted by Parkinson’s disease, according to a study published today in Nature. Parkinson’s disease (PD) is a progressive, incurable neurological disorder that often begins with subtle non-motor symptoms (e.g., sleep disturbances, constipation) and advances to disabling motor and cognitive impairments. Dysfunction of the somato-cognitive action network (SCAN)—a newly identified system coordinating arousal, visceral function, and whole-body motor planning with behavioral motivation—may underlie PD’s diverse symptoms. To investigate SCAN’s role in PD pathophysiology and treatment, we established a large multimodal imaging cohort (n = 863) spanning multiple therapeutic interventions, including medication, deep brain stimulation (DBS), transcranial magnetic stimulation (TMS), and MRI-guided focused ultrasound stimulation (MRgFUS).
Resting-state functional connectivity (RSFC) analyses revealed that the substantia nigra and all major PD DBS targets (STN, GPi, VIM) are preferentially connected to the SCAN rather than effector-specific motor areas, with PD characterized by SCAN–subcortical hyperconnectivity. Across six patient cohorts, effective treatments (DBS, TMS, MRgFUS, levodopa) consistently reduced this hyperconnectivity. In a randomized trial of 36 PD patients, repetitive TMS (rTMS) targeting the SCAN produced approximately twofold greater motor improvement compared to motor cortex targeting (week 2: ΔMDS-UPDRS-III = –13.48 vs. –6.49; P < 0.012). These findings identify SCAN hyperconnectivity as a core pathological signature of PD and demonstrate that precise SCAN-targeted neuromodulation yields superior therapeutic outcomes.
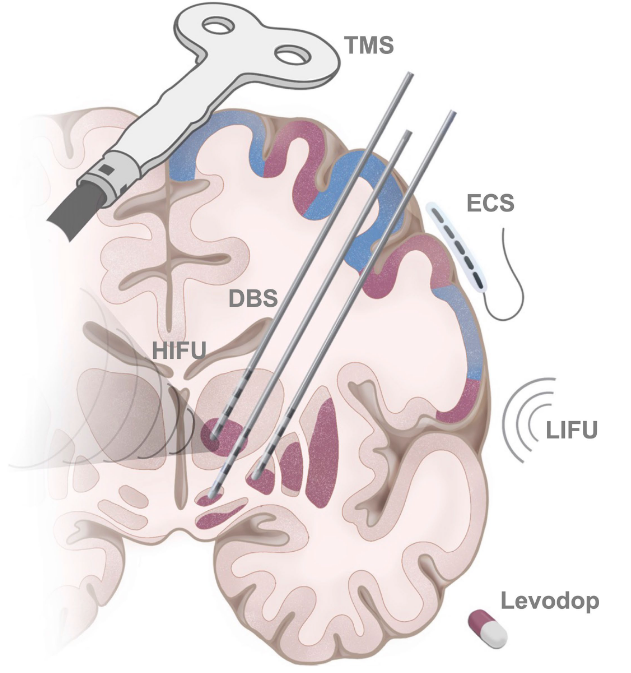
Fig. SCAN-targeted medications and neuromodulatory therapies for Parkinson’s disease.